Your Gynaecological Care
At Chelsea Gynaecology, we offer expert gynaecological care tailored to women at every stage of life. From routine examinations and preventative health checks to the diagnosis and treatment of complex conditions, our goal is to provide the highest standard care lead by Dr Shane Duffy in a supportive and professional environment.
Comprehensive Gynaecology Care
Compassionate care for a wide range of gynaecological conditions, supporting women’s health at every stage of life. We offer specialist assessment and personalised, evidence-based gynaecology treatments tailored to your individual needs.
Commen reasons patients see us
Bleeding after the menopause
If a woman has any bleeding after menopause, this needs urgent attention. After a woman has had a year with no periods, she should not bleed. We will look for the cause of the bleeding through an examination, pelvic ultrasound and if required a hysteroscopy.

Contraception methods allow you to choose when and whether you want to have a baby. We will outline all the different contraceptive methods available to you and help you decide what is the best method for you.

Endometriosis is a common condition in which small pieces of the womb lining (the endometrium) are found outside the womb. This could be in the fallopian tubes, ovaries, bladder, bowel, vagina or rectum.
Endometriosis commonly causes pain in the lower abdomen (tummy), pelvis or lower back. It may also lead to fertility problems. However, some women have few or no symptoms.
There is no known cure for endometriosis. It is a chronic (long-term) condition that can cause pain, lack of energy, depression and fertility problems. However, symptoms can be managed and fertility improved with pain medication, hormone treatment or surgery. We will tailor a management plan that will aim to reduce endometriosis interfering with your daily life.

Fibroids are benign (non-cancerous) tumours that grow in or around the womb (uterus). The growths are made up of muscle and fibrous tissue and can vary in size. Fibroids are sometimes known as uterine myomas or fibromyomas. Fibroids are common, with at least one in four women developing them at some stage in their life. They most often occur in women who are from 30 to 50 years old. Sometimes fibroids can cause symptoms, such as pain or heavy bleeding. In such cases, medication may be prescribed. If this proves ineffective, surgical or non-surgical techniques may be recommended.
Heavy periods, also called menorrhagia, are when a woman loses an excessive amount of blood during several consecutive periods. Menorrhagia is the medical name for heavy periods. Menorrhagia can occur by itself or in combination with other symptoms, such as menstrual pain (dysmenorrhoea). Heavy bleeding does not necessarily mean there is anything seriously wrong, but it can affect a woman physically, emotionally and socially, and can cause disruption to everyday life. Our assessment will screen for the causes of heavy periods:
- cervical or endometrial polyps: these are non-cancerous growths in the womb or the lining of the cervix (neck of the womb)
- endometriosis: this is when small pieces of the womb lining are found outside the womb; for example, in the fallopian tubes, ovaries, bladder or vagina
- uterine fibroids: these are non-cancerous growths in the womb that can cause pelvic pain
- intrauterine contraceptive devices (IUD), also known as ‘the coil’: blood loss may increase by 40-50% after an IUD is inserted
- pelvic inflammatory disease (PID): this is an ongoing infection in the pelvis that can cause pelvic pain, fever and bleeding after sexual intercourse or between periods
- polycystic ovary syndrome (PCOS): women with PCOS typically have a number of cysts in their ovaries
- blood clotting disorders such as von Willebrand disease
- an underactive thyroid gland (hypothyroidism): this may cause fatigue, constipation, intolerance to cold and hair and skin changes
- liver or kidney disease
- cancer of the womb (although this is very rare)

Irregular bleeding
Periods last around three to seven days. The average menstrual cycle lasts 28 days, although it’s normal to have a cycle that’s shorter or longer than this. Women’s periods can change. This doesn’t necessarily mean there’s a serious problem, but it does need to be checked. We will provide a compressive assessment and treatment plan if required.

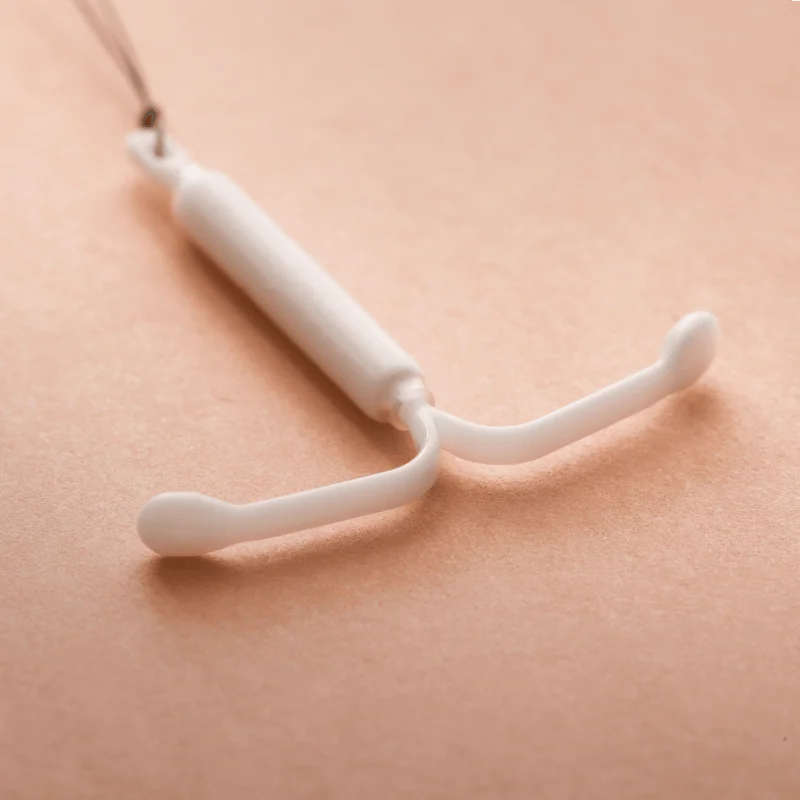
Mirena Coil
An intrauterine system (IUS) is a small, T-shaped plastic device that contains progestogen. We can insert and remove coils and IUS’. You may need to be tested for infection before the fitting or you may be given antibiotics, in case of infection, to take as it’s fitted.
An ovarian cyst is a fluid-filled sac that develops on a woman’s ovary. Ovarian cysts are very common and they do not usually cause any symptoms. If the cyst is large or is causing symptoms, it will probably have to be surgically removed. We provide a stop clinic appointment where we can diagnoses the presence of a cysts (pelvic examination and ultrasound) and outline the different surgical options available. We provide the full range of surgical options (including key hole surgery)
Painful periods, Most women experience some form of period pain (sometimes called dysmenorrhoea) during their lifetime. The medical term for period pain is dysmenorrhoea. The pain caused by menstruation is usually felt in your lower abdominal area, but can also spread to your back and thighs. We will review your symptoms, the cause of your pain and with you develop a plan to manage your symptoms.
Your period pain may be caused by an underlying medical condition. This is known as secondary dysmenorrhoea. These conditions include the following:
- Endometriosis: the cells that normally line the womb start to grow in other places within the body, usually in the fallopian tubes and ovaries. When these cells shed and fall away, they can cause intense pain.
- Fibroids: this condition occurs when non-cancerous (benign) tumours grow in the womb. They can make your periods heavy and painful.
- Pelvic inflammatory disease: your womb, fallopian tubes and ovaries become infected with bacteria, leaving them severely inflamed (swollen and irritated).
- Adenomyosis: the tissue that normally lines the womb starts to grow within the muscular wall of the womb. This extra tissue can make your periods particularly painful.
- Intrauterine device (IUD): a form of contraception made from copper and plastic, which fits inside the womb. It can sometimes cause period pain, especially in the first few months after it is inserted.
If you have secondary dysmenorrhoea, you may also have other symptoms, such as:
- irregular periods
- bleeding in between periods
- thick or foul-smelling vaginal discharge
- pain during sex

Pelvic pain
Some women can have pain in the vagina or deeper in the pelvis. This can also occur during or after sex. Pain felt inside the pelvis can be caused by conditions such as:
- pelvic inflammatory disease (PID)
- endometriosis (when womb lining grows outside the womb)
- fibroids (growths of muscle and tissue in the womb) growing near your vagina or cervix
- irritable bowel syndrome
- Ovarian Cysts
We will provide a full range of investigations to identify the cause of your pain and outline the different treatment options available to you.

Polycystic ovary syndrome (PCOS) is a condition that affects how a woman’s ovaries work.PCOS affects millions of women in the UK. There are three features which lead to a woman being diagnosed with PCOS. Even if only two of them are present, this is enough to confirm the diagnosis. The features of PCOS include:
- a number of cysts that develop around the edge of the ovaries (polycystic ovaries)
- a failure in the release of eggs from the ovaries (ovulation)
- a higher level of male hormones than normal, or male hormones that are more active than normal
These can lead to the following symptoms:
- .excessive body hair
- irregular or light periods
- problems getting pregnant (infertility)
- weight gain
- acne
- hair loss from the head
We can provide the full range of investigations (blood tests and ultrasound) and treatment options.
Sexually transmitted infections (STIs) are diseases passed on from one person to another through unprotected sex (sex without a condom) or sometimes through genital contact. We can screen and treat any infections that maybe found and provide advice on how it affects your reproductive health and how to prevent any infection in the future.

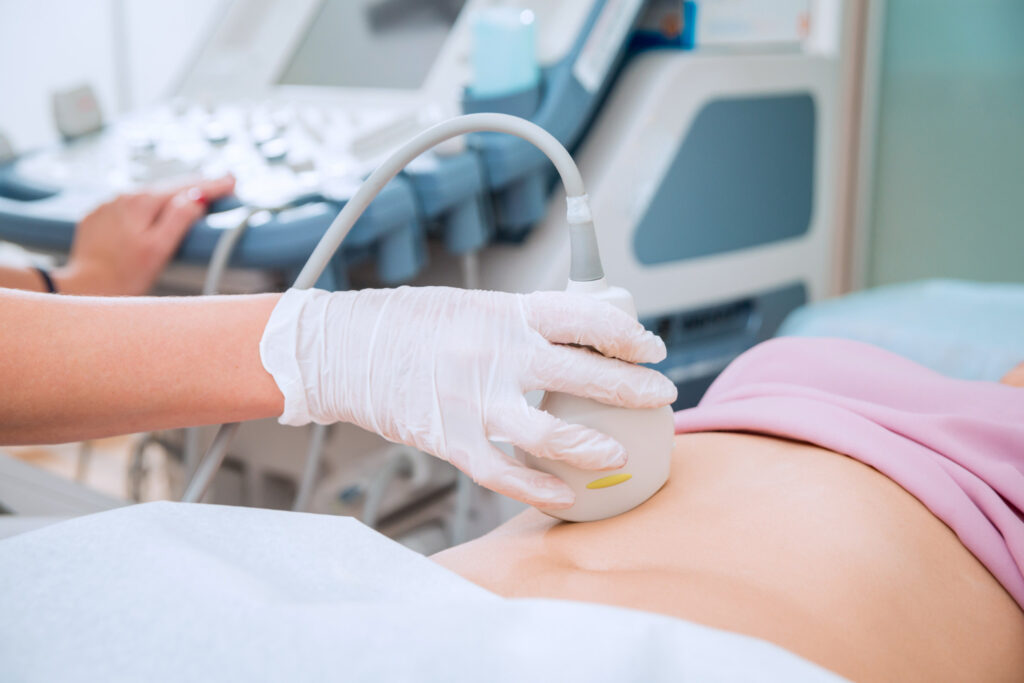
Ultrasound of the pelvic organs
This is performed for women with a variety of gynaecological complaints. The uterus, cervix and both ovaries are visualised and measured. Any cysts or abnormalities are noted. Any pathology is clearly documented. Both Consultants have extensive experience in gynaecology scanning and also get referrals from other doctors and from patients who have complex findings on previous scans.
Urinary problems
A healthy bladder is important to all of us, yet many people suffer in silence even though a lot can be done to improve things. Urinary incontinence is the unintentional passing of urine. It is a very common problem and is thought to affect more than 50 million people in the developed world. Urinary incontinence can be an uncomfortable and upsetting problem. Many people think that it is an inevitable part of ageing, but there are several forms of effective treatment. We can provide a full check of your bladder health and the full spectrum of medical and surgical treatments if needed.

Vaginal discharge
Any sudden change to your discharge may indicate a vaginal infection. You should be aware of how your discharge naturally varies throughout your cycle and what is not normal, but obvious warning signs of infection are:
- a change in colour or consistency
- a sudden bad smell
- an unusually large amount of discharge
- another symptom alongside the discharge, such as itching outside your vagina or pain in your pelvis or tummy
- unexpected bleeding from the vagina
If you are not sure whether your discharge is normal and are worried about it we can provide a full range of investigations and treatments.

Vaginal prolapse
The uterus (womb) is usually held in place by muscles, tissue and ligaments. Prolapse happens when the tissues that support the uterus become so weak that the uterus cannot stay in place and it slips down from its normal position. This can cause:
- a sensation of something coming down or out of the vagina
- an uncomfortable feeling of fullness
- difficulty having sex
- leaking a small amount of urine when you cough, sneeze or exercise
Mild cases of prolapse may not need treatment. More severe cases of prolapse may be treated effectively using a device that is inserted into the vagina called a vaginal pessary. This helps to hold the uterus in place. There are also several different surgical techniques that can be used and we are able to provide a full range of these surgical options.

Vulval problems
Alot of women experience occasional bouts of itching, irritation and swelling of the vagina and surrounding area. We will screen for the common causes of these and provide advice and treatment if necessary.

Well woman check
The check will include a medical history, lifestyle questionnaire, physical examination, pelvic scan, a cervical smear, and a consultation where you will have the opportunity to ask questions and discuss any concerns.

At Chelsea Gynaecology, we provide specialist assessment and treatment for a wide range of gynaecological conditions, including:
- Heavy periods
- Irregular periods
- Painful periods
- Polycystic ovary syndrome (PCOS)
- Menopause assessment and management
- Endometriosis
- Pelvic pain
- Fibroids
- Ovarian cysts
- Contraception and family planning
- Mirena coil insertion and management
- Sexually transmitted infection (STI) testing and treatment
- Fertility investigations
- Vaginal discharge and infections
- Vaginal prolapse
- Urinary symptoms and bladder problems
- Postmenopausal bleeding
- Pelvic ultrasound
- Perineal trauma
- Postpartum perineal tears


